Psoriasis
A Good Quality of Life with Psoriasis is Possible
With the classic presentation of psoriasis being skin that is red, inflamed, hardened, scaly, painful and flaky; it is no surprise why psoriasis patients suffer not just physically, but mentally as well when people stare or shun them in public.
However, with the right psoriasis treatment, the severity of the condition and the frequency of flare-ups can definitely be reduced, so that the patient can regain a decent quality of life and go about daily life with relative ease.
At our clinic, Dr Wong Su-Ni is a Consultant Dermatologist with over 20 years' experience—a large portion of which was dedicated to the research, teaching and treatment of psoriasis in Singapore.

Achieving Improved Skin Comfort & Appearance
See a dermatologist
Undergo a tailor-made treatment plan
Enjoy and maintain your improved skin
Schedule a consultation at 6733 3629 or drop us a message below for a skin assessment today

What Causes Psoriasis?
Usually when skin cells die, they shed away naturally and gradually that you don't even notice it, and new skin cells come to the surface. With psoriasis, however, the body speeds up the life cycle of skin cells by up to 10 times.
This means that old cells don't even have sufficient time to shed while new cells are being rapidly produced, thus they stack on top of each other. This build-up causes thickened plaque patches, which is known as psoriasis.
Psoriasis also appears to be multi-factorial. Many patients have inherited genes that make them more prone to develop psoriasis; however, other factors also seem important in triggering the onset of psoriasis. Known aggravating factors include stress, injury, irritation, infection, climate, hormonal change, drugs, obesity, alcohol and smoking.
How Common is Psoriasis?
It is a very common skin disorder worldwide, and, according to the National Skin Centre is estimated to affect 1-2% of the population in Singapore.
It affects all races, sexes, adults and children alike; though the most common age of onset is the 20s to 30s and the 50s to 60s.
It usually appears on the scalp, elbows, knees, lower back and genitals, though it can appear anywhere on the body, including the fingernails.
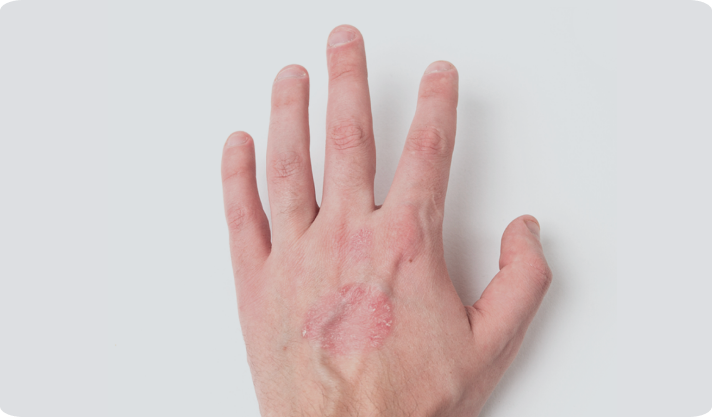
Can Psoriasis Affect Other Parts of the Body Besides the Skin?
Yes, psoriasis is increasingly being recognised as a chronic inflammatory disease that is more than skin deep.
15% to 40% of patients may develop inflammation of the joints or arthritis, which is progressively debilitating. The risk is higher in those with a family history of psoriatic arthritis or who have nail psoriasis.
Psoriasis sufferers also have a higher chance of developing diabetes, high blood pressure and heart disease.
Psoriasis Treatments We Provide
While the specific psoriasis treatment varies from individual to individual, depending on the type and severity of the psoriasis; main treatment options include:
- Moisturizers
- Topical creams and ointments
- Phototherapy with UVA or UVB light
- Photochemotherapy (PUVA)
- Oral or injectable medication (for moderate to severe psoriasis, or when joints are involved)
To schedule a consultation, please call us at 6733 3629 or drop us a message here.
FAQS
- Pustular psoriasis Small pus-filled blisters with surrounding redness and swelling of the skin; may be localized to the palms or soles.
- Erythrodermic psoriasis Generalised red, swollen, scaly skin—often a preventable complication of untreated or improperly treated psoriasis.
- Guttate psoriasis Small, drop-like, scaly lesions over the body; commonly seen in children and young adults.
- Flexural psoriasis Smooth red lesions in the folds of the skin; commonly seen in the groin, armpits and under the breast.
- Palmo-plantar psoriasis Red, scaly patches of skin affecting the hands and feet only, and often mistaken for hand and feet eczema.
- Scalp psoriasis Psoriasis localized to the scalp, where it causes profuse dandruff. A proportion of these may develop into psoriasis elsewhere after a few years.
- Psoriatic Arthritis In addition to the skin, psoriasis can also affect the nails and joints.


